CHPW’s Procedure Code Lookup Tool lets you search for services by procedure code and line of business to determine:
- If a prior authorization (PA) is required (indicates “yes” or “no”)
- If there are PA conditions
- If the service is a covered benefit (indicates “covered” or “not covered”)
- The benefit requirements (limits, frequency, etc.)
- Whether clinical review is needed
- Specific clinical criteria CHPW applies and documentation needed for prior authorization (PA) review
Please note:
- The Procedure Code Lookup Tool is not intended to replace the use of the Prior Authorization list, nor is the tool necessarily complete. Providers should only use this tool as a supplement to and after first consulting the Prior Authorization lists.
- If you select the Washington Apple Health Behavioral Health Services Only (BHSO) plan, the lookup tool provides PA and coverage information for behavioral health benefits only. Medical benefits for BHSO members are not administered by CHPW.
- For Medicare Advantage, refer to local coverage determinations (LCD) and/or national coverage determinations (NCD) for full clinical criteria.
- For additional benefit information, see the Member Benefit Grids:
- Apple Health Integrated Managed Care and BHSO, https://www.chpw.org/providercenter/prior-authorization/.
- Medicare Advantage, including supplemental benefits (acupuncture, naturopathy, dental, meals, ride share, etc.), https://medicare.chpw.org/provider-center/provider-resources/. Some of these services are defined by provider specialty rather than procedure code, or are services covered outside the claims system, and therefore will not be listed within the tool.
- Cascade Select, https://individualandfamily.chpw.org/provider-center/provider-resources/.
See also the “Examples” section at the end of this bulletin.
Accessing the Lookup Tool
Please make sure to check the existing Prior Authorization lists first, then check the lookup tool at https://forms.chpw.org/pclt in addition to the PA lists:
- Medicaid: https://www.chpw.org/provider-center/prior-authorization/
- Medicare Advantage: https://medicare.chpw.org/provider-center/prior-authorization/
- Cascade Select: https://individualandfamily.chpw.org/provider-center/prior-authorization/
Questions?
If you have questions about the Procedure Code Lookup Tool, please email Customer Service at [email protected].
Examples
Here are some examples from the tool.
Home Page
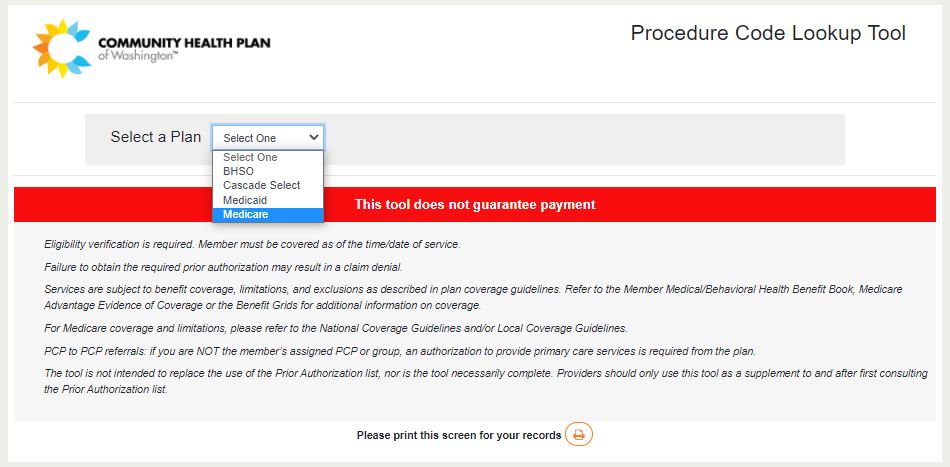
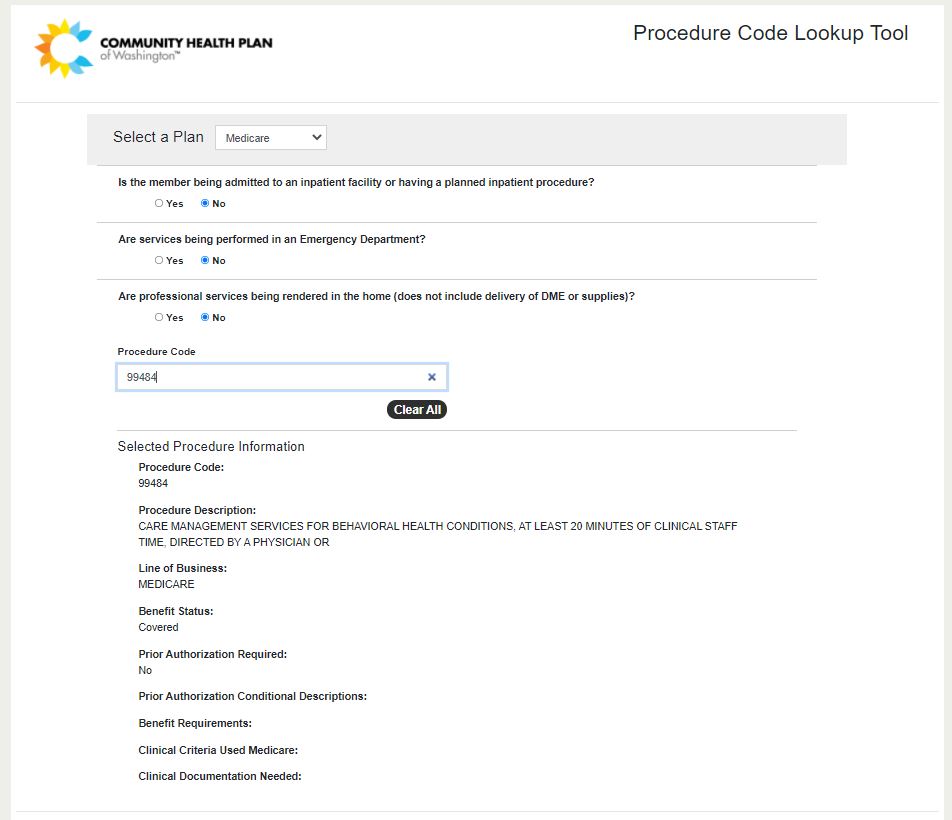
Medicare Plan
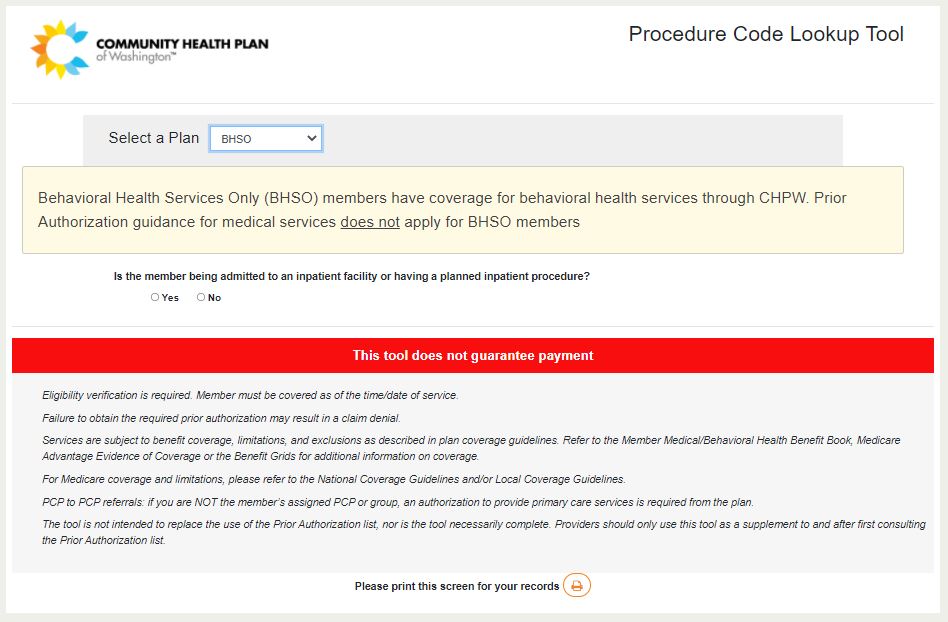
Behavioral Health Services Only (BHSO) Plan


 Many Americans do not get enough sleep and this can contribute to a number of health issues. Taking a nap during the day can help your body restore itself and promotes brain and heart health. A 20-minute nap has a variety of health benefits – from improved mood, to better focus and memory function. In some cultures, napping is even prescribed as a health treatment by doctors!
Many Americans do not get enough sleep and this can contribute to a number of health issues. Taking a nap during the day can help your body restore itself and promotes brain and heart health. A 20-minute nap has a variety of health benefits – from improved mood, to better focus and memory function. In some cultures, napping is even prescribed as a health treatment by doctors!