Medicare Advantage metrics
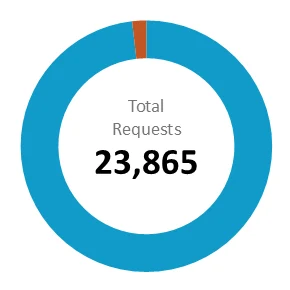
Standard prior authorization (Non-urgent)
|
Approved after timeframe was extended 20,878 /22,398 |
Average time (mean) 165.65 hrs |
|
Approved after appeal 234 /435 |
Median time (middle) 140 hrs |
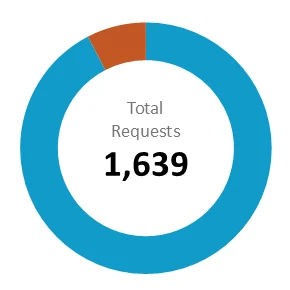
Expedited prior authorization (Urgent)
|
Approved after timeframe was extended 63 /1,514 |
Average time (mean) 29.39 hrs |
|
Approved after appeal 21 /43 |
Median time (middle) 5 hrs |
Methodology and definitions
Data source and reporting period
All prior authorization data is sourced from Community Health Plan of Washington (CHPW). Metrics reflect final authorization decisions recorded during the prior calendar year.
Prior authorization priority classification
Requests are categorized based on their recorded priority at the time of submission:
- Standard (Non-Urgent): Reported as classified in the system
- Expedited: Reported as classified in the system
- Urgent: Counted as Expedited for reporting purposes
Scope of services
This report includes non-drug medical prior authorization requests across all service categories, including:
- Inpatient services
- Outpatient services
- Durable Medical Equipment (DME)
- Other non-prescription medical services
- Prescription drug prior authorizations are excluded from this report
Lines of business
Metrics include all Lines of Business (LOBs) administered by Community Health Plan of Washington during the reporting period. No LOBs are excluded unless otherwise noted in supplemental materials.
Decisions status definitions
Reported metrics reflect final decision outcomes for each authorization request:
Approved: Requests fully approved as submitted
Denied: Requests denied in full
Partially Approved: Counted as Denied for reporting purposes
Excluded administrative outcomes
To ensure that reported denial rates reflect meaningful clinical determinations, certain administrative or non-clinical outcomes are excluded from denial counts. Requests with the following Decisions are filtered out:
- Duplicate
- No PA required
- Data entry error
- Requested in error
- Void
- Withdrawn



